The Architecture of Imaging: The Design of the Radiology & Imaging Sciences Department
Introduction to Design Considerations
Medicine is a science, but the practice of medicine is an art. This is especially true in the branch of medicine called medical imaging. The art of applying medical imaging requires high-technology equipment, tremendous care and patience, and a unique sensitivity.
Imaging facilities are often viewed as simply places for high technology equipment. However, the fact that imaging equipment may cost considerably more than the enclosure surrounding it should not detract from the human aspects of the imaging environment. It is vital that design professionals do not focus on technical requirements so closely that they forget the needs of the people who will use that technology. One way to prevent technology from overpowering design is for the architectural team to thoroughly understand both the processes and the equipment used for medical imaging and for the medical team to understand how the design process will be orchestrated.
What are the special features of an imaging facility? It must accommodate the special needs of imaging patients and their families; the needs of the imaging staff including radiologists, technologists, other health care providers, administrators, clerical personnel and housekeeping; and the needs of the equipment in terms of its function, installation, maintenance, modification and replacement.
The Needs of Patients
Patients have many needs, some of which are for information, stress reduction, comfort, dignity, and privacy. Most patients come to an imaging department to “solve a medical mystery.” Ultrasound, magnetic resonance, computed tomography, or any one of a number of other imaging modalities offer special abilities to “see within” and visualize what would otherwise be invisible. This information needs to be precise. In terms of facility design, the equipment needs to installed properly so that it yields reliable and accurate results. It also means that user capacity must be considered to ensure that patients have access to the equipment they need in a timely manner.
In addition to this, patients have a great need for stress reduction. The diverse array of machinery is foreign and even frightening to most patients. The odd postures patients must assume, the duration for which they must hold still and the overall sense that their health and well being may be determined in part by an electronically rendered illustration of their inner anatomy and physiology can be, at best, impersonal and intimidating. At worst, it can be terrifying. Patients are very apprehensive about what the machines will say about them.
Patients need to be as comfortable as possible while waiting. Those undergoing nuclear medicine techniques may need to ingest radioactive substances before their scans, and those waiting for ultrasound scans may require to drink large quantities of water. Patients often feel a sense of alienation, and waiting areas should be large enough to permit family members to wait with them.
Patients need to maintain a sense of dignity. They need privacy to remove their clothing, and they appreciate it when private offices and public spaces are acoustically treated to prevent their conversations from being overheard. Patient privacy is also enhanced when acoustic separation of patient and staff areas restricts the sound of business within work areas.
The Needs of Staff
Imaging is an “information hub” of medicine. Staff members need precise, timely medical information. For example, imaging facilities must provide staff members with ready access to medical records, test results, scheduling and billing information, and so on. Additionally, staff need adequate storage space.
Factors that enable imaging staff to perform their duties efficiently are:
- Task lighting should be appropriate and adequate
- Size and configuration of treatment rooms should facilitate their function
- Needs of housekeeping and maintenance personnel must be addressed
- Imaging staff have stressful work, and need break rooms and private areas and appreciate pleasant conditions as much as patients do.
The Needs of Equipment
As imaging equipment becomes more computer based, the need for “clean” and uniform power and efficient air-conditioning systems is magnified. Infrastructure systems designed by engineers must be carefully coordinated with architectural design.
Because medical technology is changing at an increasingly rapid rate, the need for flexibility in every aspect of design becomes more crucial. Alternatives for future growth and modifications should be part of the initial design, not an afterthought.
Finally, although imaging equipment itself is shrinking in size, the capabilities of any single piece of equipment are expanding. As a result, multiple ancillary instruments may be used in the exam room. Therefore, the need for both examination space and support space may increase.
Department Location & Configuration
The numerous activities surrounding an imaging examination intertwine to form a complex, almost choreographed sequence of events. For hospital based imaging departments, the department location and configuration must be coordinated with the hospital-wide flow of patients, staff, supplies and material.
Department Location & Access
Frequently, imaging departments are located on the ground floor of the hospital. Major parts of the department may not have access to natural daylight. The weight of imaging equipment and film files and desired adjacencies to other departments frequently located on the lower levels (such as the emergency department and the outpatient department) are some of the reasons that make this ground floor location necessary. This grade-level location is preferred for this department. It can accommodate the need for future expansion. This ability to expand the department or to allow for future conversion of areas within the department should be a primary consideration in determining location and configuration.
Where the imaging department should be located within the hospital depends on two factors:
- Who will be using the departments services
- What the facilities overall organizational philosophy is with regard to the provision of imaging services
Users of Imaging Services
Imaging services often comprise of at least three components: basic imaging, special imaging and nuclear imaging. Basic imaging includes routine procedures (for example, basic radiology and fluoroscopy) that are of short duration and frequent demand. Special imaging includes procedures (for example, magnetic resonance imaging (MRI), computed tomography (CT) and interventional imaging) that are of longer duration and often require specialized equipment. Nuclear medicine is a unique form of imaging that measures radiation emitted from an internal source of radioactivity. Sometimes all three components are organized to form a central imaging department. Sometimes basic imaging is decentralized whereas special imaging and nuclear medicine are centralized; and sometimes nuclear medicine is organized as a separate department. Additionally, in some cases, special zones within the department are dedicated to certain patient groups- for example, a women’s screening area with ultrasound, mammography and bone densitometry.
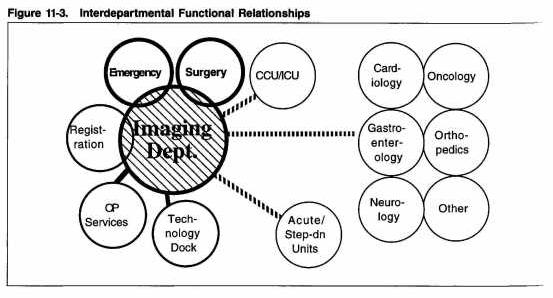
Adjacencies required for a centralized imaging department (see: figure) include:
- Outpatient registration and clinic areas
- The emergency department
- The surgical suite
- Nursing units
Access from Outpatient Areas
Because more imaging functions are performed on an outpatient basis, ambulatory patients make up an increasing majority of imaging procedures. In many cases, outpatients will be required to have chest X ray, blood work and an electrocardiogram (ECG) prior to other form of outpatient treatment. Basic x-ray services, as part of an outpatient imaging facility or the main imaging department should be near the OPD. Imaging services should also be easily accessible to specialty clinics, such as orthopedic clinics (which frequently use general radiography, MRI and CT), obstetric/gynecological clinics (which use ultrasound) and oncology clinics (which use many imaging modalities such as MRI, CT, radiography, fluoroscopy, mammography, ultrasound, and nuclear medicine).
Access from the Emergency Department
Emergency patients often need immediate access to many imaging services, especially basic radiography, CT and MRI. Most large ED’s (20,000 or more annual visits) have some imaging capabilities within the department. Despite this, close proximity to the imaging department is desirable to improve access to specialty imaging services that are integral to ED care. Additionally, if some imaging services are not staffed at night, the ED may be the only area that is fully staffed. Thus, if the ED is located on the ground floor, ideally imaging services should also be located there.
Access from Surgery
Imaging is becoming an increasingly important component of surgery, and surgical procedures are becoming an increasingly larger component of imaging. Presurgical planning, which utilizes three-dimensional CT and MRI, is useful in the preparation for complex surgical procedures. Various forms of imaging such as ultrasound, fluoroscopy, and even CT also are significant tools used within the operating suite to track surgical progress and location. Imaging itself is becoming more interventional. Surgical procedures such as stereotactic neurosurgery or biopsies may be performed within CT or even MRI suites.
Many imaging procedures now involve invasive treatment, and thus some imaging procedure rooms may require a high level of sterility and additional support spaces for additionalpersonnel and patient observation and holding. Imaging integral role in surgery requires that(1) radiologists and technologists need access to surgical suites and (2) surgeons will be performing more procedures in conjunction with imaging personnel. Thus both proximity and advanced communication systems between the two departments is desirable.
Imaging’s interventional nature suggests that some patients may need surgical backup in the event of a medical emergency. In addition, observation of imaging patients prior to and after their procedures can sometimes be effectively combined with the end-stage observation of surgical outpatients.
Access from Nursing Units
As inpatient census declines and much of the emphasis of health care shifts to outpatient diagnosis and treatment, the patient population in the hospital is generally more critically ill than it was in the past. Thus, imaging plays a pivotal role in the management of inpatients.
In the intensive care unit (ICU), in particular, rapid turnaround of images and image interpretation is essential to the effective care of patients because their medical condition is likely to change quickly. In addition, it is important to minimize transport of these patients. One approach is to process, interpret and hold ICU patient’s images within the ICU for the duration of the patients stay in the unit. Another alternative to help accomplish these goals would be a partial picture archiving and communication system (PACS), connecting the ICU to a centralized imaging department.
The imaging department should have direct access to and from elevators used for inpatient transport.
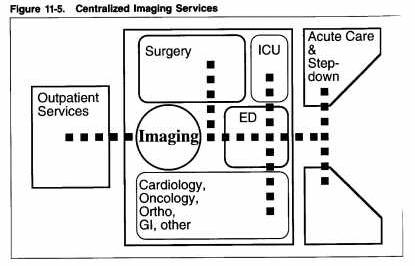
Centralized versus Decentralized Imaging Services
An institutions decision to centralize or decentralize imaging services within the hospital is related to that organizations overall philosophy of providing medical care. For centralized departments, where both basic and specialized imaging services are located within one zone, vertical and horizontal connections to the various users of imaging services will be necessary.
In contrast, sometimes hospital imaging functions are decentralized and organized around specialty programs. Decentralized imaging usually results in duplication of routine imaging equipment, which is located close to inpatients, in addition to a centralized imaging department, where specialized imaging procedures are performed. For example, nursing units and diagnostic and treatment functions may be organized by individual organ-specific or medical subspecialty program floors, such as muscoloskeletal programs (providing orthopedic, rehabilitation and radiology services), neurosensory programs (providing neurology, neurosurgery and neuroradiology services), and cardiopulmonary programs (providing cardiac and thoracic surgery, cardiology, pulmonary and radiology services). Organization based on decentralized programs is often found in large teaching hospitals where patients, staff, interns, and medical students would otherwise have to frequently travel long distances between related areas.
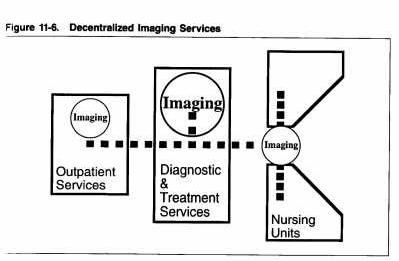
Decentralized imaging is also part of the patient-focused health care delivery strategy to reduce the amount of inpatient transport, to simplify the radiography work flow process, and to reduce overall labor costs. Another form of decentralized imaging occurs when outpatient imaging is separated from inpatient imaging.
Proponents of centralized imaging claim that in a centralized department, quality control is monitored better, radiology personnel are utilized more effectively, and equipment is not duplicated unnecessarily. On the other hand, advocates of decentralized imaging cite reduced patient transport, decreased waiting time, reduced overall labor costs, a streamlined imaging workflow process, and flexibility as beneficial outcomes of decentralizing these functions.
Decentralized imaging suggests a decentralized system of filing and scheduling that makes patient data accessible wherever they are needed. Decentralized active film can further complicate what traditionally has been one of the most problematic areas of imaging departments- keeping track of patient records and diagnostic images. Decentralized scheduling can also complicate the orderly and efficient utilization of procedure rooms. However, both these processes are areas where electronic PACS and image management and communication systems (IMACSs) can be real assets once they become more cost-effective.
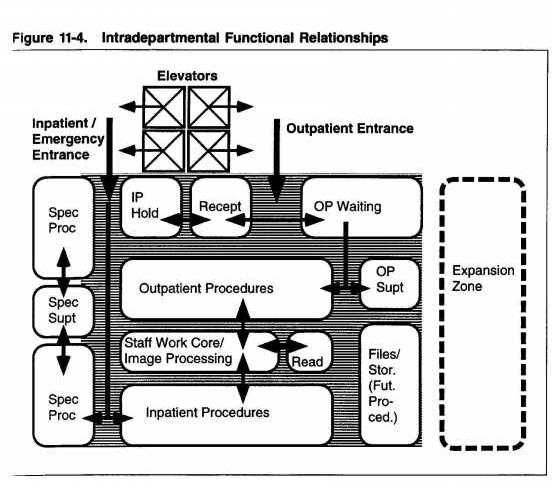
Department Configuration: The Functional Zone Concept
Numerous systems based on repetitive planning modules have been used to develop the layout of imaging departments. One notable example is a detailed system of modular radiology planning described in 1972 by Dr. Thure Holm of the University Hospital in Lund, Sweden, at the International Symposium of Planning of Radiological departments in Finland. This concept, sometimes referred to as the functional (or concentric) zone concept, was further described in 1982 by Dr. Harry Fisher of Strong Memorial Hospital-University of Rochester (New York) School of medicine and Dentistry. It comprises of the following activity zones:
- Patient zone, where waiting and patient preparation occur
- Examination zone, where the primary activity of imaging examination occurs
- Central image-processing zone, where the three functions of image handling occur
- Personnel zone, where staff offices and support spaces are located
- Long-term file zone, where inactive files are stored
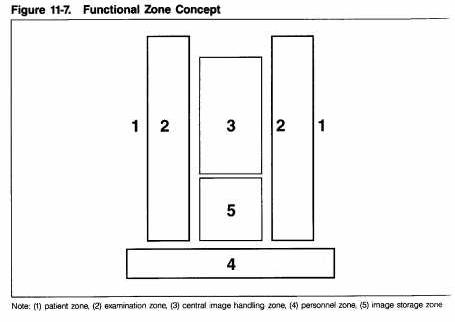
Although details of Holm’s and Fisher’s descriptions of modular planning are somewhat dated (for example, room sizes will not necessarily apply to today’s equipment and electronic image management was not considered because it was not yet available), the philosophy behind the concept is worthy of review. Their identification of separate functional zones led to a clear planning logic that has since been incorporated into many contemporary design solutions.
Patient Zone
The patient zone includes space for patients prior to and after their imaging procedure(s). Patients have their first contact with the imaging department and staff in this area. First impressions should be positive ones.
If both inpatients and outpatients are seen in the department, the patient zone can be separated into two distinct areas, each adjacent to the examination zone. Functions found in the patient zone include:
- Patient and visitor waiting areas
- Dressing rooms
- Toilet rooms
- Lockers
- Education space
- Reception and registration areas
- Patient corridors
- Patient preparation and holding areas
Reception and registration should be provided such that clerical staff can easily supervise waiting areas and have easy access to patient records and administration areas. A room or alcove screened from the waiting area should be provided for confidential or financial conversations and/or as an education space.
Sometimes, dressing rooms are clustered together, with each cluster serving a series of procedure rooms, rather than locating a dressing room near each procedure room. A clustered arrangement tends to accommodate variations in workflow and thus more effectively maintain a high volume of patient examinations. Clustered dressing rooms may also accommodate the accessibility requirements for disabled people more efficiently than do segregated dressing rooms. If clustered dressing rooms are used, the design should preclude patients from having to travel far through public corridors to and from procedure rooms.
Examination Zone
The examination zone consists of two primary elements: examination or procedure rooms and control areas. Both patients and staff enter the examination zone. Patients are limited to the procedure room and the patient side of the registration area; they are not permitted in the control area.
The control area is where technologists’ consoles and other equipment used to “control” the imaging procedure are located. In the functional zone concept, all control functions were removed from the procedure room and placed in a control corridor, running parallel to a series of procedure rooms.
In many facilities, however, the preferred location for control alcoves is within the procedure room. This occurs more often in basic procedure rooms than it does in special procedure rooms. Special procedure rooms often have a large control room directly adjacent to the procedure room, rather than within a control corridor. There are advantage and disadvantages to both.
The imaging department should be arranged such that those procedures that are of short duration and high frequency are located near the waiting area and the department entrance. This configuration will thus reduce the amount of traffic congestion in the patient corridor.
Image-Processing Zone
Imaging departments that have been planned using the functional zone concept often have a staff work core in the center. If the control corridor approach is used, the work core abuts the control corridor. If the control corridor approach is not used, the work core abuts procedure rooms that have internal control alcoves and control rooms adjacent to the procedure rooms.
The image-processing zone provides space for three functions:
- Image processing, quality control and preliminary viewing, where the image is processed and reviewed for quality prior to being sent to the radiologist
- Reporting and consulting, where the radiologist reviews and interprets the image for diagnosis and/or consults with the referring physician or others
- Film sorting and short-term film storage, where active images are sorted and stored for archiving (active status may last for months or even years)
In some practices, reporting and consulting are performed in the personnel zone instead of the image-processing zone.
Personnel Zone
The personnel zone includes office space and staff support areas such as lockers, toilet rooms, lounges and conference spaces. If staff lounges and conference are to be shared by other departments, these spaces should be located along the perimeter of the department to keep non-departmental traffic away from busy work areas.
Many radiologists review and interpret images in their offices; others review and interpret them in multi-viewing rooms complete with film alternators, film illuminators and multimedia computer workstations that integrate PACS, IMACS and RIS (radiology information system), and HIS (hospital information system) capabilities.
Long-Term File Zone
Various regulatory bodies have rules regarding the length of time inactive films must be retained, as well as individual practice philosophies. It is not uncommon for films to be archived for seven years or longer. Inactive film storage often can be located in an area remote from the main department, providing that some means of retrieving old films is practical.
Plan Typologies
Over the years, the size and configuration of imaging facilities has evolved in parallel with the evolution of health care facilities and imaging equipment. This section discusses a variety of common plan typologies. Many corridor-based typologies, which lack flexibility, reflect the configuration of early hospitals with long single- and double loaded corridors. Core and cluster plans improve on their more linear predecessors and reflect an approach to planning that is more appropriate.
Single-corridor imaging department layouts developed as a result of long, narrow hospital wings. Although these layouts may be suitable for small departments with small workloads, the single-corridor plan has many limitations.
First, inpatient, outpatient, staff and service traffic are combined. In addition, there is often little separation between departmental traffic and through traffic. Expansion is inconvenient and usually limited to one end, and travel routes are long.
The traditional double- loaded corridor plan is a slight improvement over the single- corridor arrangement. Although there is potential for some traffic segregation, travel distances are still long. Communication among staff and the mixing of different types of traffic remain a problem. In addition, space utilization tends to be inefficient because the increased amount of corridor space is disproportionate to the limited functional advantages it provides.
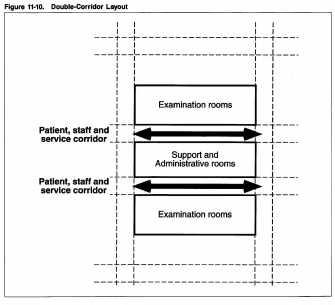
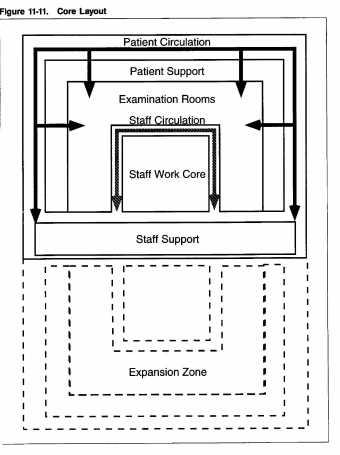
The core plan solves some of the inefficiencies found in the single- and double-corridor layouts. Based on a concentric arrangement of activity zones, the core plan separates staff and patient areas and allows for the separation of inpatient and outpatient traffic.
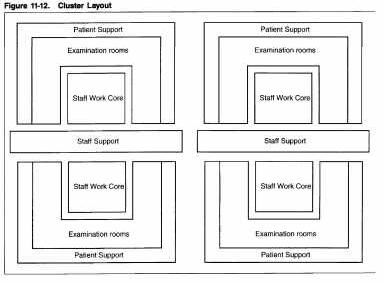
The cluster plan is a modified form of the core arrangement. Cluster plans allow for separation of activity clusters within the examination zone. For example, basic radiography, special radiography, mammography, and ultrasound activity clusters can all be made accessible in a cluster arrangement. This is beneficial when separate zones for special patient groups are desired. In addition, a cluster arrangement usually can accommodate aphysical link between the imaging department and a separate imaging dock or relocatable imaging unit.
Cluster plans are ideal for most medium- and large-size facilities. They usually accommodate multiple image-processing and viewing areas without creating long travel distances for patients and staff.
Space Requirements
Planning for too much space costs a lot of money; planning for too little costs even more! With all the complexity and continually changing variables associated with medical imaging, how is it possible to determine the size of an imaging facility, to determine the number and size of procedure rooms needed and their optimum configuration? Because all facilities are unique, there is no single answer to a question such as “how big is a radiology department?” any more than there is an answer to “How big is a house?”
Determining space requirements is a rigorous and complex process that depends on the outcome of other related studies, such as strategic analysis and functional programming. A broadbrush approach may be acceptable at a projects inception when no more than order-of-magnitude information is needed to see whether it is financially viable, to continue detailed planning without verifying preliminary guesstimates is inappropriate.
This section describes a general methodology for determining space requirements for any imaging facility and identifies the variables that influence the size of a particular institution. Discussion includes how to project the type, number and size of procedure rooms required, as well as the amount and size of support space required. It implies a careful analysis of a facilities needs.
Space Determinant Methodology for the Imaging Facility
Planning for the space requirements of an imaging facility requires interaction among facility planners and facility users. Two processes – functional programming and space programming – must precede the design and planning stages. Functional programming evaluates historic and present workload data in order to calculate future projections. Thus, functional programming is the first step in the umbrella process of programming. Its end product describes anticipated workloads (quantity, duration and mix of procedures) in terms of staffing, equipment and workflow. Space programming translates the functional program into area requirements. It includes a list describing the size, number and spatial characteristics of every room and department in the facility.
Space programming begins with a series of interviews among planners and the administrative and medical users of the facility during which the planning team collects and reviews data, projects anticipated workloads, and calculates requirements. Following are the key components involved in those activities:
- Data Collection (provided by facility users in case of an existing facility)
->Existing workload in terms of procedure mix and quantity
->Existing staffing requirements
->Existing equipment requirements
->Historic workload data to determine past trends (where applicable)
->Degree of satisfaction with existing space, equipment and facility
- Workload projections (determined by functional programming team in conjunction with facility users)
->Assumptions regarding future trends, based on operational goals, market changes and changes in technology
->Future workload in terms of procedure mix and quantity
->Staffing projections to accommodate future workload
->Equipment projections to accommodate future workload
- Space and functional requirements (determined by programming and planning team in conjunction with facility users)
->Area requirements to accommodate future workload (number and size of rooms to accommodate anticipated patient examinations, consultations, treatment, and so on)
->Area requirements to accommodate future staffing
->Area requirements to accommodate future equipment
->Area requirements to accommodate future expansion
->Functional adjacencies
->Work flow and traffic patterns
The user group interviews will disclose varying opinions from different individuals within the organization (administrators, radiologists, technologists, nurses, physicists, engineers, housekeeping personnel, clerical staff, patient advocates, and so on). Because the most vocal individuals may not necessarily be those with the most authority, recording individual requests without obtaining some degree of consensus from the group can prove misleading. Thus, the planning team will benefit from having one key individual from each user group first take responsibility for reviewing and verifying the collected data and then become part of the review process all the way through the contract documents and construction phases of service.
Key Space Generators
For each type of room or area, there is usually a primary generator, or key space generator, that best determines its number, size and shape. Key space generators include units of work (for example admissions per year), number of staff and size of equipment.
However, some types of room are affected by more than one key space generator. For example, the optimal number of radiographic rooms is determined primarily by the anticipated number of annual exams, whereas each room’s size and shape are influence by the array of equipment and how it will be used. An additional key space generator for a radiographic room in a teaching hospital having the same equipment as its community hospital counterpart might be the need to provide additional space for observers of, or participants in, a procedure.
In contrast to radiographic rooms, which are sized according to workload and equipment requirements, offices are sized according to the number of occupants and their importance within the organization, the number of people involved in consultations, how the office is used, and, therefore, the size and arrangement of furniture. Workload (the number of consultations) has little influence on office size. The number of offices required is based on staffing, which is indirectly a result of both workload and number of procedure rooms. In teaching facilities, the number of offices may be higher than in non-teaching facilities.
Types of Space
Most imaging facilities are composed of three types of space: activity, support and administration. Activity space reflects the primary activity of the facility and is the key determinant of department area.
The size and configuration of imaging rooms are often determined by clearances required for the specific imaging equipment selected. room dimensions are further influenced by patient flow, staff flow, and ancillary equipment that will be used within the room.
Support space and administration space directly assist the function of activity spaces, whose characteristics determine their number and size. For example, control rooms assist the functions of CT scanning rooms. The number and size of control rooms and computer rooms are determined by the type and quantity of CT equipment, the anticipated CT workload, and the number of staff and equipment in the control room. Similarly, administration space (office and clerical area) requirements are determined by the number and type of staff needed to support and operate the imaging equipment and to assist imaging patients.
Activity Clusters
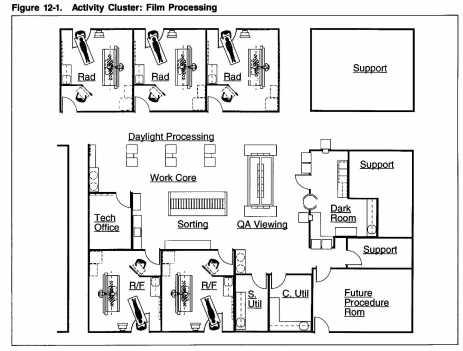
In most instances, certain types of spaces are grouped together in what can be called an activity cluster. The individual spaces in the activity cluster work together to support various functions. In the case of film processing, a darkroom (or daylight processing area), an image quality viewing area and a film sorting area form an activity cluster. Separate tasks are performed within each space, and yet if one of the spaces is not provided, the entire film-processing activity cannot be accomplished. Thus, a film processing room is usually supported by a viewing area to verify image quality before the patient dresses again.
A film-processing activity cluster can be centralized (supporting many procedure rooms), decentralized (supporting a select group of rooms with imaging equipment that can all share the same type of processor), or dedicated (located within the procedure room and attached to an individual piece of imaging equipment). When film processing occurs in the procedure room, image quality can be checked without a separate viewing area. With some image acquisition techniques such as MRI and CT, image quality is reviewed on computer monitors.
Other examples of activity clusters include:
- Fluoroscopy room/toilet room (so that patients can eliminate immediately following the exam in the event barium enemas are used)
- Ultrasound room/toilet room (so that patients undergoing abdominal ultrasound can eliminate large quantities of water consumed prior to the exam)
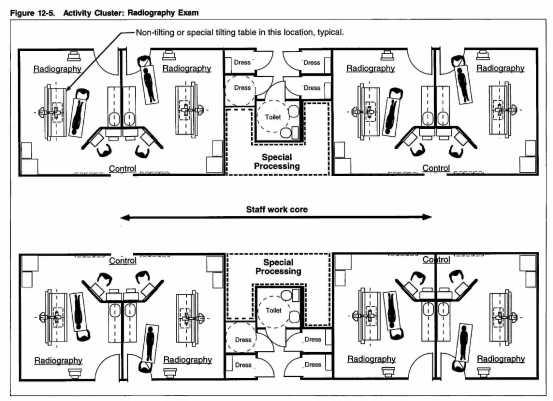
- Radiography room/control room/dressing area
- CT scanning room/patient prep and holding/ control
- Nuclear medicine scanning room/toilet/dressing/holding dose room
- Positron emission tomography (PET) scanning room, cyclotron/dose room
Variables Affecting Facility Size
The following variables should be considered while determining facility size:
- The number of annual operating hours differs among institutions. Workload projections must be based on stated assumptions regarding operating hours per day and operating days per year. Additionally, at most hospitals the imaging workload varies dramatically from one shift to another. The night shift has peaks and lulls, depending on the workload of emergency cases. In contrast, the day shift may be heavily scheduled and will be subject to staff efficiency and the frequency of emergency cases disrupting the schedule.
- Renovation projects are likely to require more space then a newly constructed facility with the same workload capacity, because planning may not be able to be as efficient as with new construction.
- If radiographic facilities exist in the emergency department, they should not be counted as part of the primary emergency workload. However, radiology staffing may be inefficient if the same personnel are used to staff the two departments.
- Although some imaging equipment is getting smaller, many imaging procedures are becoming more complex and more people and ancillary equipment are involved; thus, some room sizes are getting bigger and additional patient holding areas are required. Equipment throughput capabilities are increasing; thus in some instances, the number of annual procedures per examination room is getting larger. Automated image processing and image management and communication systems can reduce average procedure durations, thus also increasing the number of annual procedures per examination room.
- Imaging workload is determined by the type of patients in an institution and not just the number of patients. For example, a hospital with a large obstetrics program is likely to perform more abdominal ultrasound examinations than one without a significant number of such patients. Similarly, a major heart center is likely to do more cardiac imaging than a hospital that does not focus on cardiology. Magic numbers that simply convert patient beds to procedures per year do not reflect the fact that all patient beds are not equal.
- Outpatient imaging centers, as compared to hospital imaging departments, are likely to perform more routine procedures of short duration. Thus an outpatient facility is likely to accommodate more procedures per room per hour than a hospital. However, the outpatient facility may not be open as many days per week or as many hours per day as a hospital department. Thus each room may accommodate relatively fewer procedures per year as compared to hospital procedure rooms.
- Some institutions include nuclear medicine as a part of radiology, others do not. Some even include radiation therapy as a part of the radiology department. Some institutions have MRI within the imaging department; some have MRI in a separate facility or modular enclosure. A clear description of what is to be included in the department is necessary before determining department size.
- Some institutions have one central imaging department; others decentralize routine imaging rooms and locate them near the various inpatient units nursing units. Special procedure rooms are usually placed within one central location. Some institutions combine inpatient and outpatient imaging; others have two 9or more) separate facilities. Each of these variables will influence the amount and type of space needed.
- Archival film files are frequently stored in a location that is remote from the main imaging department or even off-site. Department area calculations will be affected by whether remote file storage is included or excluded from the total area calculation.
- Filmless imaging departments may eventually require less space for film files than film-based imaging departments. Filmless imaging departments eventually may require less space than film-based departments for image reading and interpretation workstations, although initially more space will probably be required, because both film-based and filmless workstations will co-exist until the latter becomes fully integrated into daily routines. Therefore, the degree to which a department utilizes filmless imaging technology will influence space requirements.
Room Design
Room design is closely related to the both the people who use the room and the equipment that is used in it. There are many possible design approaches. Like the imaging department itself, each room must be designed in concert with workflow; patient, staff and support traffic; and the spatial perceptions of the individuals using the room. Additionally, primary design drivers, or key space generators for many rooms, are the placement, size, movement and access requirements of individual imaging modalities.
Below are given some basic criteria to be considered when planning a radiographic procedure room. The intent is not to describe every room component in detail nor is it to describe any single best design solution for the room in question, but rather to provide general guidelines. To do this for every type of room in the typical imaging department would be beyond the scope of this lecture.
General Considerations for Procedure Rooms
Because the complexity and characteristics of many procedure rooms are evolving rapidly, the number of personnel in the procedure room and the acuity of patients are increasing. And because the size, sophistication, type and quantity of equipment to be found in many rooms are changing equally rapidly, the dimensions, physical characteristics and infrastructure requirements of some rooms are not necessarily fixed. This applies more to special procedure rooms, such as angiography and catheterization labs, than is does to most basic procedure rooms, such as general radiography/fluoroscopy (R/F) rooms.
Formulas for complex procedure room design are of limited value. Even those for basic procedure rooms need to be modified for single-corridor, double-corridor, core, or cluster department configurations. See the discussion on Plan Typologies above. The combining or separation of patient and staff traffic will alter the number of entrances (and hence the layout) of the procedure room in question.
The ability of staff to easily observe patients is another key consideration affecting room design. For example, the technologist should be able to see the patient’s face at all times from the control area. If the patient table is accessible only from one side and tilts from horizontal to vertical, this establishes a physical relationship between the placement of the control area and the placement of the patient table within the procedure room. In addition, if the radiologist (or invasive cardiologist) needs access to the patients right side, an unobstructed view of ceiling- supported monitors, and the assistance of others who can reach catheters and other supplies with minimal movement at the same time that the technologist in the control area needs an unobstructed view of the patient and the physician, the equation becomes more complex. Maximum lengths of pre-assembled equipment cables also influence room design.
Trends
Two trends regarding imaging processing rooms are worth noting here. The first is that the complexity of outpatient imaging procedures continues to increase. The second is that, many procedures, both inpatient and outpatient oriented, are becoming more invasive.
Facility implications of the increasing complexity of outpatient procedures are numerous, especially for facilities other than acute care hospitals. First, floor -to-floor heights in non-hospital buildings are traditionally lower than they are in hospitals. The ability to construct functional and flexible procedure rooms without adequate vertical clearance may be compromised where vertical clearance is inadequate. Similarly, power, heating, ventilation and air- conditioning (HVAC), plumbing and fire-fighting systems typically designed for non-hospital buildings may be inadequate for complex procedure rooms and their equipment. Separate systems may be required just for the imaging component of some outpatient facilities. Structural systems in non-hospital facilities must be able to support the load created by imaging equipment. Additional structural reinforcing may be needed for outpatient renovation facilities. Floor-loading capacities that are greater than for other types of non-hospital buildings may be needed for new construction.
The implications of increasingly invasive imaging procedures are also numerous. Some procedure rooms require higher levels of infection control, greater emergency and uninterruptible power supply, emergency equipment, medical gas outlets, and more space than was previously required. To accommodate infection control criteria, special wall floor and ceiling finishes may need to be specified. Special methods of assembling these materials to limit the growth of organisms and to simplify cleaning procedures also may be necessary. In addition, exhaust, ventilation, and air-filtration specifications may need to be upgraded for these procedure rooms.
Details
A broad array of fixtures and accessory equipment is needed in most procedure rooms. Some notable examples follow:
- A hand-washing fixture should be provided in the room.
- Some special procedure rooms need to have scrub sinks located nearby.
- Some rooms, such as cardiac catheterization labs, need an additional sink located nearby for cleaning catheters.
- Many procedure rooms that emit radiation require that that patients and personnel wear lead-lined aprons or other forms of protective clothing. Therefore apron racks are required in or near those rooms. Additionally, radiation protection is integrated into the room construction itself.
- If conventional film processing is used, a lighttight through-the-wall cassette pass-box should be installed, ideally directly between the control portion of the procedure room and the darkroom.
- Film illuminators of the proper orientation and configuration should be placed where they are accessible for easy viewing.
Coordination of the numerous accessory items and fixtures required in the procedure room should begin early in the design development phase. If it is not, last- minute decisions regarding seemingly minor items can severely compromise a workable procedure room layout. Wall thickness should be increased where flush mounted accessories are used and where major conduits pass through wall partitions. Usually, it is advantageous to increase the wall thickness around the entire procedure room.
Future Trends
In the 1970’s and much of the 1980’s, long-range planning established an integral foundation for the design and construction of most healthcare facilities. However, as the eighties and nineties progressed, the duration of planning horizons shortened noticeably, as healthcare delivery systems began to reflect changes in healthcare reimbursement, notably, the advent of managed care and cost containment. At present, even short term planning forecasts are qualified with great risk and uncertainty.
This uncertainty during an era of rapid change requires that today’s planning be done in such a way as to accommodate many possible outcomes. Although the details of tomorrow’s health care environment are unclear, it is possible to determine a general direction.
Following is a look at the impact of changes in the health care reimbursement and delivery system in the area of medical imaging:
- A shakeout or survival of imaging modalities with high-outcome-to-cost ratios, while less efficacious techniques struggle for reimbursement
- Increased requirements to justify the economic value of new modalities
- An increased reliance on predetermined clinical pathways or courses of action for patient care
- The increased volume and complexity of outpatient imaging services
- A decreased cost per imaging procedure
- Improved cost accounting and pricing required by capitation
- The development of telemedicine and teleradiology as integral components of health care delivery
- Volatile political debates surrounding outcome monitoring as a means of directing the future growth of specific imaging modalities
- Cross-trained healthcare technicians performing technical tasks that were previously performed exclusively by imaging technologists
- An increased development of interventional imaging procedures, including imaging applications in the operating room.
Design Goals
The architecture of imaging facilities reflects the humanistic, technical, social and economic characteristics of health care in general being described in this workshop on healthcare design. As in the design of any complex facility type, functional concerns must be integrated with the physical image that is intended for the facility.
Yet healthcare architecture in the 21st century is certain to have a different emphasis than it has had in the past. As healthcare functions in an area of cost containment, there may be a tendency among some to devaluate the importance of facility image and favor the economic criteria by which facility design is judged. However, a sounder approach is to consider that health care is changing it’s focus from a treatment-based industry to one of both prevention and treatment. In this regard, image and ambiance are better judged in terms of both their cost and contribution to health and well being than in terms of cost alone.
Phew!
If you reached this point, you are to be congratulated on your powers of perseverance. I guess you learned more about imaging facility design than you ever thought necessary. What if I were to tell you that the above represents only a small fraction of the book it was cadged from? Anyway, peace.
I hope it comes in of use. In the end, it is a question of understanding and then applying common sense in the context of your design skills. Hang in there!
————————————————————————————————————————————————————————
Source: The Architecture of Imaging by Bill Rostenburg, AIA – American Hospital Publishing
Hussain Varawalla: Healthcare Architect – Can be reached at
hussain@healthcarearchitecture.in
204 thoughts on “The Architecture of Imaging: The Design of the Radiology & Imaging Sciences Department”